Testing your blood sugar level is one of the best ways to understand your health and how different foods, medications, and activities affect it. Keeping track of your blood glucose can help you and your doctor makes a plan to manage your best health, and your diabetes if you have it.
People use portable blood glucose meters, called glucometers, to check their blood sugar levels. These work by analyzing a small amount of blood, usually from a fingertip. For some, how to use these tools is as normal as an inhale or an exhale, while for others new to this scene, this is a great overview to set your foundation of knowledge. And now? There are Continuous Glucose Monitoring Systems, or CGM’s.
A CGM automatically tracks your glucose levels day and night using a small sensor worn on the back of the upper arm and a monitor that lets you view your glucose levels at any time. Unlike a blood glucose monitor, which only gives you a current glucose reading, CGM shows additional insights into where your glucose level was, currently is, and where it’s headed – and can even share that information with us so we can support you!
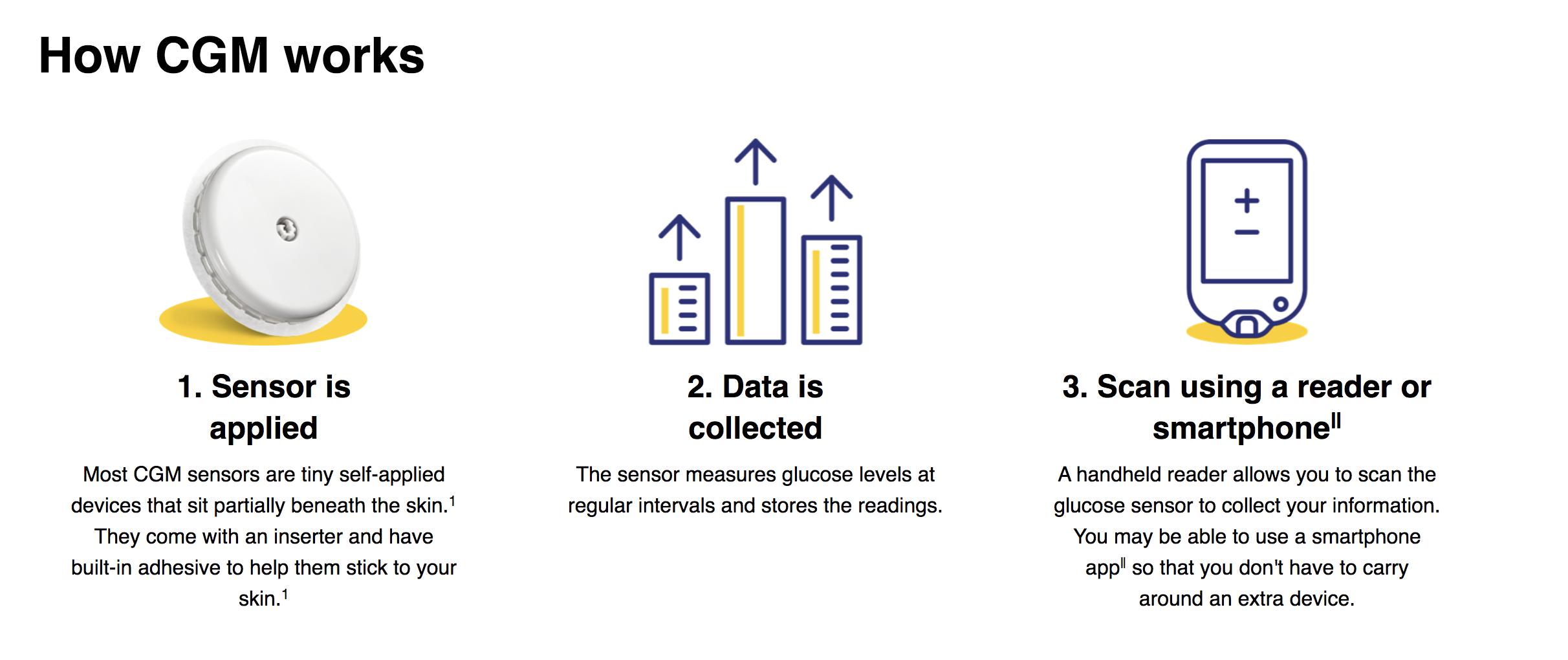

Read on to learn more about blood sugars and levels overall – and then let’s talk!
Questions? Book your appointment with us and we will walk through your every option and answer your every question.
Regular blood sugar monitoring is the most important thing you can do to manage type 1 or type 2 diabetes. You’ll be able to see what makes your numbers go up or down, such as eating different foods, taking your medicine, or being physically active. With this information, you can work with your health care team to make decisions about your best diabetes care plan. These decisions can help delay or prevent diabetes complications such as heart attack, stroke, kidney disease, blindness, and amputation. Your doctor will tell you when and how often to check your blood sugar levels.
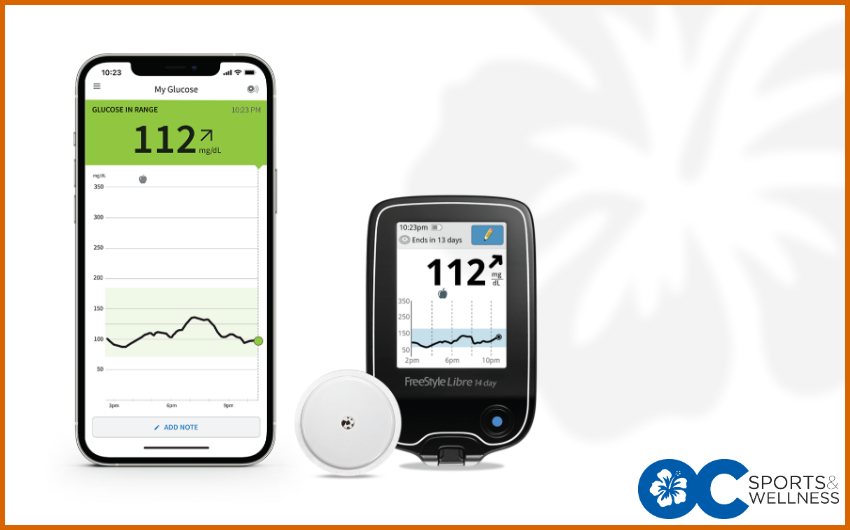
Most blood sugar meters allow you to save your results and you can use an app on your cell phone to track your levels. If you don’t have a smartphone, keep a written daily record like the one in the photo. You should bring your meter, phone, or paper record with you each time you visit your health care provider. Here’s an idea of how a CGM such as Freestyle Libre can appear.
How to Use an (Old School) Blood Sugar Meter
There are different kinds of meters, but most of them work the same way. Ask your health care team to show you the benefits of each. In addition to you, have someone else learn how to use your meter in case you’re sick and can’t check your blood sugar yourself.
Below are tips for how to use a blood sugar meter.
- Make sure the meter is clean and ready to use.
- After removing a test strip, immediately close the test strip container tightly. Test strips can be damaged if they are exposed to moisture.
- Wash your hands with soap and warm water. Dry well. Massage your hand to get blood into your finger. Don’t use alcohol because it dries the skin too much.
- Use a lancet to prick your finger. Squeezing from the base of the finger, gently place a small amount of blood onto the test strip. Place the strip in the meter.
- After a few seconds, the reading will appear. Track and record your results. Add notes about anything that might have made the reading out of your target range, such as food, activity, etc.
- Properly dispose of the lancet and strip in a trash container.
- Do not share blood sugar monitoring equipment, such as lancets, with anyone, even other family members. For more safety information, please see Infection Prevention during Blood Glucose Monitoring and Insulin Administration.
- Store test strips in the container provided. Do not expose them to moisture, extreme heat, or cold temperatures.

Recommended Target Ranges
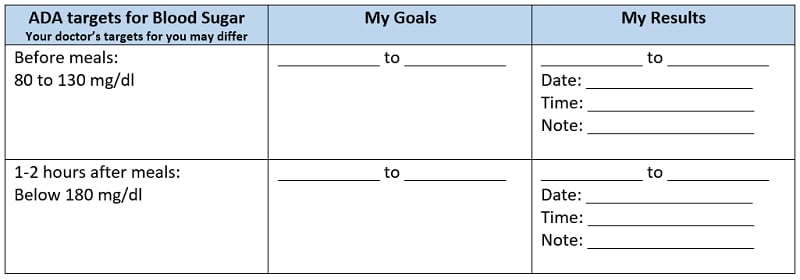
The following standard recommendations are from the American Diabetes Association (ADA) for people who have diagnosed with diabetes and are not pregnant. Work with your doctor to identify your personal blood sugar goals based on your age, health, diabetes treatment, and whether you have type 1 or type 2 diabetes.
Your range may be different if you have other health conditions or if your blood sugar is often low or high. Always follow your doctor’s recommendations.
Below is a sample record to discuss with your doctor.
Getting an A1C Test
Make sure to get an A1C test at least twice a year. Some people may need to have the test more often, so follow your doctor’s advice.
A1C results tell you your average blood sugar level over 3 months. A1C results may be different in people with hemoglobin problems external icon such as sickle cell anemia. Work with your doctor to decide the best A1C goal for you. Follow your doctor’s advice and recommendations.
Your A1C result will be reported in two ways:
- A1C as a percentage.
- Estimated average glucose (eAG), in the same kind of numbers as your day-to-day blood sugar readings.
If after taking this test your results are too high or too low, your diabetes care plan may need to be adjusted. Below are ADA’s standard target ranges:

Benefits of CGM
Glucose readings without fingersticks
Rather than taking glucose readings from your blood, CGM sensor readings are taken from interstitial fluid, a thin layer of fluid that surrounds the tissue cells below your skin. As carbohydrates are digested, glucose enters your bloodstream before it is absorbed into the interstitial fluid.
See trends and patterns to help better manage diabetes
CGM gives you a view of your glucose levels over time; it can help you keep track of past glucose levels and provide insights into future trends.
Think of glucose readings as the cars of a train, where the front of the train is blood glucose and the back of the train is sensor glucose. Because glucose enters the bloodstream first, blood glucose readings lead sensor glucose readings. Eventually, sensor glucose readings catch up to blood glucose readings just like the back of the train following the front of the train. BGM provides a glucose value for the specific point in time when a blood drop is read, whereas CGM gives you a more complete picture of where your glucose is going, and where your glucose has been, so you can make more informed treatment decisions.
The insights from CGM can help you figure out what has triggered a spike or a drop in glucose levels, such as exercise or something you ate.”Right away I started wanting to modify my behavior to get better results.” – Vykki, CGM User
Questions To Ask Your Doctor
When visiting your doctor, you might keep these questions in mind to ask during your appointment.
- What is my target blood sugar range?
- How often should I check my blood sugar?
- What do these numbers mean?
- Are there patterns that show I need to change my diabetes treatment?
- What changes need to be made to my diabetes care plan?
- Is a CGM right for me?
If you have other questions about your numbers or your ability to manage your diabetes, make sure to work closely with your doctor or health care team.
Reference: {https://www.cdc.gov/diabetes/managing/managing-blood-sugar/bloodglucosemonitoring.html & https://www.freestyle.abbott/us-en/what-is-cgm.html}
Do you want access to Direct Primary Care and less expensive, personalized healthcare that offers so much more than you probably know even was an option? Learn more on our Facebook page HERE or call us at 949.460.9111 and let’s talk.
If we can be of service in any way, or if you’d like to ask us questions on our Direct Primary Care and memberships, please reach out!
At OC Sports and Wellness you can actually text or video-chat your doctor, as well as schedule a visit. Let’s talk! 949-460-9111




